CONTEXT
With the continuing surge of COVID-19 cases in India, there has been a significant increase in the generation of biomedical waste (BMW). The Central Pollution Control Board (CPCB) recorded the generation of 710 metric tonnes (MT) of biomedical waste per day, as of May 31 2020. Of this, 101 MT/day was COVID-related biomedical waste from hospitals, quarantine wards, sample collection centres and testing laboratories [1]. Before the pandemic, both private and government hospitals typically generated 500 gram of BMW per bed each day, which has now risen to about 2.5-4 kg per bed [2].
It is imperative to point out that in the present scenario, along with Health Care Facilities (HCFs), households are generating a considerably high amount of BMW. Such waste is classified as ‘domestic hazardous waste’ by the Central Pollution Control Board (CPCB). PPE kits, face masks/shields, and gloves, among other protective equipment, are made from plastic and are neither biodegradable nor fit for recycling. Moreover, the unscientific disposal of BMW, along with the contagious nature of the virus, can result in biohazards with detrimental environmental and health impacts.
PRESENT BIOMEDICAL WASTE MANAGEMENT SCENARIO
On July 17, 2020, the CPCB issued the fourth revision of guidelines on the handling, treatment and disposal of biomedical waste of COVID-19 patients [3]. These are an extension to the Bio-medical Waste Management (BMWM) Rules 2016, the most comprehensive guidelines for the scientific disposal of solid and liquid BMW at both the institutional (healthcare facilities, quarantine centres, among others) and individual (quarantine homes and containment areas) levels. All stakeholders, including Urban Local Bodies (ULBs) and Common Biomedical Waste Treatment and Disposal Facilities (CBWTFs) need to comply with the Rules. However, the implementation of these guidelines during the pandemic becomes a larger concern, as gaps have been identified in the on-ground compliance with BMWM Rules.
In 2018, as per the annual report by the State Pollution Control Boards (SPCB) and Pollution Control Committees (PCCs), there were 27427 instances of violations of the BMWM Rules 2016 reported against healthcare facilities and CBWTFs [4]. Given this context, the ongoing pandemic has aggravated the severity of the challenges that the Indian waste management system deals with, some of which are discussed below.
SEGREGATION AND DISPOSAL
The guidelines issued by the CPCB stress on segregation of BMW at the source, not only for its effective handling but also to avoid contamination which can adversely affect public health. Table 1 lists the categories for segregation and treatment of BMW under the 2016 Rules.
Table 1: Segregation and Disposal of COVID-19 Biomedical Waste
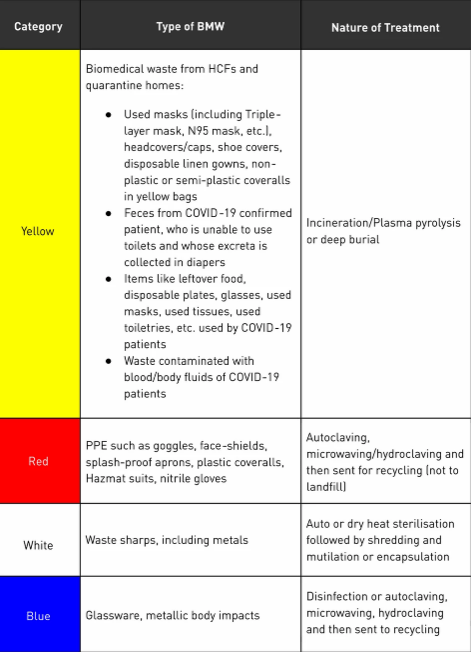
The National Green Tribunal (NGT) Status Report highlights the rise in improper segregation of biomedical waste from COVID-19 isolation wards, quarantine centres and quarantine homes [5]. All isolation wards for the diagnosis and treatment of COVID-19 patients are to segregate their waste into different colour-coded bins or bags as mandated in the BMWM Rules 2016. However, WHO in its 2017 report, titled ‘Healthcare Waste Management Status in Countries of the South-East Asia Region’, stated that 72% of India’s hospitals do not segregate their waste and only 50% ensure daily waste collection by the authorised CBWTF [6]. Swati Singh Sambhyal, a UN waste management expert, highlights that only 70% of the BMW produced in India gets treated in incinerators and 30% of it is either illegally dumped or found as common garbage on the roads [7].\
While ULBs may provide colour-coded yellow bags for hazardous COVID waste and handle it from quarantine homes, there is a lack of segregation etiquette followed in Indian households. For instance, an uninfected mask or glove needs to be shredded and should be wrapped in paper for 72 hours before its disposal as general waste [8]. There have also been incidents of mix-ups of BMW from containment zones and safe localities [9][10][11]. The absence of general awareness among people and waste collectors of requisite segregation rules has the potential to lead to severe ecological and health hazards. The mixing of biomedical waste with general solid waste jeopardises the efficiency of incinerators, which are not designed to treat general domestic waste, resulting in the production of excessive emissions and unburnt ash.
ROLE OF URBAN LOCAL BODIES
ULBs play a crucial role in training sanitation workers and monitoring the safe and scientific disposal of BMW. While some states have designated private agencies for waste collection and deployed vehicles till the CBWTFs, others have given these responsibilities entirely to CBWTFs.
ULBs are required to certify that biomedical waste is lifted immediately by the authorised CBWTF from hospitals and isolation centres [12]. They need to provide yellow colour-coded bags to quarantine homes and ensure door-to-door collection of household medical waste by trained waste workers or CBWTFs directly. However, how much of that mandate is actually being fulfilled by ULBs is up for debate. Generally, ULBs are supposed to provide bins to households to ensure compliance with source segregation practices, but there is evidence suggesting a failure to adhere to these guidelines [13][14].
Experts like Satish Sinha, Associate Director of Toxics Link, have suggested that instead of ULBs training separate workers for the collection of BMW, the task can be handled by the CBWTFs alone as the nature of the waste remains the same whether produced in hospitals or households [15]. However, citizens often raise objections when BMW collection vehicles enter their neighbourhoods due to the threat of disease and the stigma associated with the virus [16]. According to the guidelines and the BMWM Rules 2016, household hazardous waste could also be deposited at collection centres by its generator, but its actual implementation remains compromised because of the absence of such centres [17].
The guidelines also authorise ULBs to designate a nodal person who is to be responsible for feeding daily data in the ‘COVID-19 BMW Tracking App’. But as per the information submitted by the SPCBs/PCCs, only 15 states and UTs have implemented the functioning of this app, increasing the disparity in the monitoring of waste [18]. The analysis presented in the WHO report states that some SPCBs acknowledge the absence of accurate data as most of it was based on extrapolation because of significant monitoring loopholes within the system [19].
FACILITY CRUNCH AND IMPACT
As per the CPCB annual report, currently India has 200 CBWTFs which are operational for the treatment and disposal of BMW (generally for BMW generated in HCFs), excluding five states/UTs (Andaman and Nicobar Islands, Arunachal Pradesh, Goa, Mizoram, Nagaland and Sikkim) which have nil. Besides this, 15281 HCFs have captive treatment facilities (installed in the absence of CBWTFs within 75 km of the HCFs). The NGT Status Report states that 55% of the cumulative incinerator capacity has already been utilised by the states [20]. India had an inadequacy of infrastructural treatment capacity even before the pandemic. With coronavirus cases having crossed the four million mark, BMW disposal has become an even more serious challenge. The available disposal capacity and the number of cases recorded seem to be proportional to each other. This is represented in the table below with the top 3 states having the maximum number of confirmed positive cases.
Table 2: Utilised waste disposal capacity in states producing maximum BMW as of May 31st, 2020
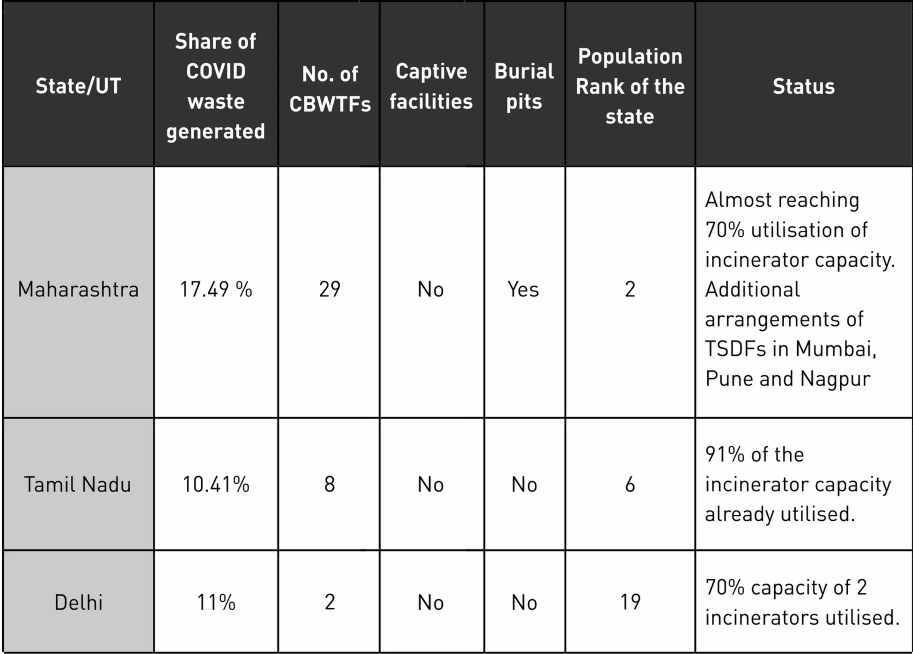 SOURCE: NGT Status Report 2020, 2011 CENSUS, MOHFW
SOURCE: NGT Status Report 2020, 2011 CENSUS, MOHFW
Approximately 50% of the states and UTs have inadequate disposal facilities. States with the utilisation of 70% of the total incinerator capacity are the ones that also have the highest positive cases recorded [21]. Due to the lack of segregation practices and technological upgradation of machinery, most of the waste is burnt in incinerators leading to the generation of toxic gases hazardous to workers and people’s health living around these facilities.
In case of generation of BMW where the requisite disposal facility is unavailable, the CPCB guidelines permit the use of at least 100 feet-deep burial pits as a last resort. However, 80% of states and UTs have not provided information on the formulation or implementation of a model plan for the disposal of BMW in villages or subdivisions [22]. Moreover, the WHO report quoted earlier states that 56% of the BMW is dumped openly, and complaints have been received over illegal dumping in agricultural lands [23]. Practices like these affect soil health and lead to contamination of groundwater, making it unfit for drinking. According to the WWF, if 1% of all masks are disposed of incorrectly, it could result in 10 million masks per month dispersed in the environment [24]. Such cases have been reported in Maharashtra where heaps of used masks, gloves, syringes and other protective equipment were found dumped on beaches [25]. Conservationists have warned that the pandemic is leading to a new environmental crisis.
CONCLUSION
The COVID-19 pandemic has laid bare the insufficiency embedded in the waste management system in India. Realising this situation, the government under Prime Minister’s Science, Technology and Innovation Advisory Council (PMSTIAC) invited individuals, start-ups and entrepreneurs to the “Biomedical Waste Treatment: An Innovation Challenge” in July 2020 to come up with sustainable social engineering solutions [26]. Though the results of the challenge are yet to be released, the policy response to the management of BMW cannot be restricted to reactive measures in the wake of the pandemic. Challenges in segregation, transportation, and treatment capacities for BMW were present at a functional level even before the pandemic. The unsustainable nature of biomedical waste disposal practices has only increased the chances of an additional ecological and health hazard at present. The current situation is, thus, a wake-up call that must lead to stricter monitoring of BMW management at the institutional level as well as behavioural interventions at the household level.






